The vascular system is something most people don’t think about until something goes wrong.
 The vascular system is how blood moves throughout your body. The heart pumps blood to your lungs, which oxygenate the blood. Then the heart sends the oxygenated blood to muscles and organs throughout the body by way of your arteries. Your veins are what bring that blood back to your heart. More often than not, even those with healthy hearts and lungs can have trouble with imperfect vein function. It’s estimated that 30 to 60 percent of adults have varicose veins.
The vascular system is how blood moves throughout your body. The heart pumps blood to your lungs, which oxygenate the blood. Then the heart sends the oxygenated blood to muscles and organs throughout the body by way of your arteries. Your veins are what bring that blood back to your heart. More often than not, even those with healthy hearts and lungs can have trouble with imperfect vein function. It’s estimated that 30 to 60 percent of adults have varicose veins.
“When I was a 16-year-old athlete, I noticed a bluish lump on the back of my calf. My mother shook her head and said, ‘I’m sorry—you got that from me.’ Of course, I assumed it was a weird bruise—something that would go away. But it was the beginning of my first varicose vein,” said Sarah Ison of Arlington. “For me, because it started so early, I can only blame heredity. That vein now stretches down to my ankle and up the back of my knee. Sometimes it aches and throbs, at other times it doesn’t bother me. I’m 44 years old now and I’ve always hated the way my veins looked, but I’ve been hesitant to treat them. I watch my weight and other risk factors. But soon, I know I’ll have to do something about it, I just don’t know what. I keep putting it off.”
What are Varicose Veins?
According to the National Institute of Health, varicose veins are swollen and twisted veins that are formed when weakened valves allow blood to pool and back up in your veins. As with Sarah Ison, sometimes varicose veins are caused by heredity. Other risk factors are aging, obesity, pregnancy, blood clots or trauma, and standing or sitting for long periods of time. Symptoms can include a feeling of fullness or heaviness, throbbing discomfort and pain, visible swollen veins, evening leg cramps, and mild swelling in the ankles.
Not only are varicose veins unsightly, they can be uncomfortable and painful. Over the years, treatments have improved the outcomes for people choosing surgical options.
What about Spider Veins? What can I do?
Spider veins are dilated capillaries just under the surface of the skin. Although harmless, they are visible on the legs and sometimes the face. Studies show that as high as 84 percent of the population has some form of spider veins. Showing up as a web of red and blue across the skin, the good news is that there are simple cosmetic treatments to treat them, and sometimes, to eliminate them.
What are Surgical Options for Varicose Veins and Spider Veins?
 Treatments for varicose veins are considered medical and not cosmetic by most physicians and insurance companies. Spider veins are considered a cosmetic procedure and can be treated by a cosmetic surgeon, a dermatologist, a phlebologist or vein specialist, an interventional radiologist, or a vascular medicine doctor or vascular surgeon. Check with your doctor about your options. Here are some of the latest treatments.
Treatments for varicose veins are considered medical and not cosmetic by most physicians and insurance companies. Spider veins are considered a cosmetic procedure and can be treated by a cosmetic surgeon, a dermatologist, a phlebologist or vein specialist, an interventional radiologist, or a vascular medicine doctor or vascular surgeon. Check with your doctor about your options. Here are some of the latest treatments.
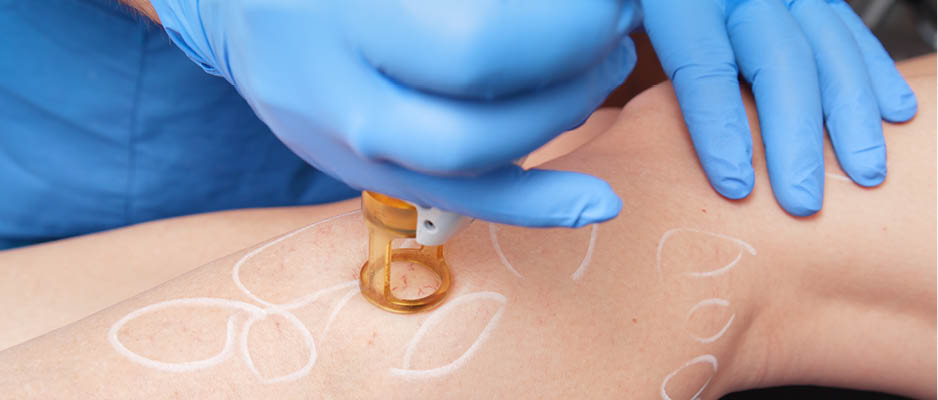
- Lasers and Intense Light—surface lasers such as Vasculight and Photoderm are options for spider veins and blue veins called reticular veins. By using highly focused beams of light that damage the varicose veins or capillaries, scar tissue forms and closes down the vein, allowing the blood to reroute using other, healthier veins.
- Sclerotherapy—although this treatment has been around since the 1930s, it’s still considered highly effective on both mild varicose veins and spider veins. A solution that dissolves the vein or capillaries is injected directly into the vein. It can be performed in the doctor’s office and sometimes takes four to six treatments. Compression stockings are needed after sclerotherapy sessions.
- Ambulatory Phlebectomy—for more severe varicose veins, ask your doctor about a phlebectomy. In this surgical procedure, large surface veins can be removed through very small incisions that don’t require stitches. Most patients return home the same day as the procedure. Most doctors today prefer the phlebotomy over earlier procedures such as vein stripping. It has a higher success rate, has less bruising, and gives a quicker recovery time. After a phlebectomy, expect to wear heavy compression stockings for several weeks and expect mild discomfort and bruising while your body heals.
- Endovenous Thermal Ablation (ETA)—some varicose veins are connected to a broken large vein in the thigh called the great saphenous vein (GSV). Removing varicose veins without addressing the GSV in the thigh can lead to treatment failure. With ETA, a catheter is inserted into the bad thigh vein near the knee and threaded up. Once in position, the catheter tip is activated. The tip heats the inside lining of the vein as the catheter is slowly withdrawn. The intense heat seals the bad GSV internally and closes it, reducing the risk of future varicose veins.
What can you do besides surgery to improve the appearance and discomfort of varicose veins and spider veins?
- If obesity is a factor, talk to your doctor about weight lose options
- Do not sit or stand for long periods of time
- Whenever possible, elevate legs above the heart to minimize discomfort
- Get more exercise, including weight training and walking
- Wear compression stockings prescribed by your doctor
- Avoid wearing high heels and clothing tight around the waist and groin area
As with any other procedure, educating yourself with your options is the first step in choosing treatment. Don’t wait for your mild discomfort to turn into pain. Treat your varicose veins and spider veins just as you would the rest of your vascular system: with care. Healthy veins make for a healthier you!
By Susan Ishmael









